Conquering Insulin Resistance: Hormonal Balance through Low Carb Diets
Conquering Insulin Resistance: Hormonal Balance through Low Carb Diets
Welcome to an insightful journey into understanding and managing insulin resistance, a silent challenge faced by many midlife women. As our bodies transition through menopause, hormonal imbalances often lead to insulin resistance, affecting our health and lifestyle. This article delves into the role of low carb diets in combating insulin resistance and promoting hormonal balance.
Understanding Insulin Resistance
Insulin resistance occurs when your body’s cells are unable to effectively use insulin to absorb excess blood glucose produced from the food you consume. As a result, your liver converts this surplus glucose into fat. This condition often leads to weight gain and can contribute to a cycle of sugar cravings and addiction. Understanding this condition is the first step in addressing it effectively.
Insulin Resistance and Hormonal Changes in Midlife Women
Menopause brings significant hormonal shifts that can impact insulin sensitivity. The reduction in estrogen levels is linked to decreased insulin sensitivity, making midlife women more prone to insulin resistance. This section explores how these hormonal changes directly affect insulin dynamics in the body.
Insulin resistance due to various factors other than menopause and diet. These include:
Physical Inactivity: Sedentary lifestyles contribute significantly to the development of insulin resistance. Regular physical activity helps improve insulin sensitivity.
Age-Related Changes: As women age, they naturally lose muscle mass and gain abdominal fat, both of which can increase insulin resistance.
Genetic Factors: Genetics play a role in the predisposition to insulin resistance. A family history of type 2 diabetes or other metabolic conditions can increase the risk.
Hormonal Imbalances: Apart from menopausal changes, other hormonal imbalances, such as thyroid disorders, can impact insulin sensitivity.
Stress: Chronic stress leads to the release of hormones like cortisol, which can contribute to insulin resistance.
Sleep Disturbances: Poor sleep quality or sleep disorders, including sleep apnea, are linked to increased insulin resistance.
Medications: Certain medications, including steroids and some psychiatric drugs, can affect insulin sensitivity.
The Impact of Insulin Resistance
Insulin resistance can lead to a variety of health challenges, including type 2 diabetes, cardiovascular disease, and weight gain. It can also exacerbate menopausal symptoms like hot flashes, mood swings, and fatigue. Understanding these impacts helps in recognizing the importance of managing insulin resistance.
How do you know if you have insulin resistance?
You can check your insulin levels next time you do your yearly blood work. A fasting insulin of greater than 5.0 may be an early sign of insulin resistance.
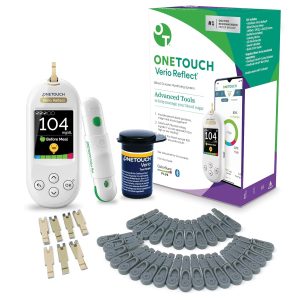
Check your own insulin levels. You can easily find a glucometer at any local pharmacy such as Target, CVS, Walgreens, or online, and you don’t need a prescription to buy one. One popular and reliable brand is OneTouch, which offers the OneTouch for under $50 on Amazon. That’s my personal choice for daily use.
This glucometer comes with lancing device, lancets, and test strips.
Many glucometers include a few test strips, but you’ll likely want to purchase additional strips in the future to monitor your blood sugar over several weeks. Remember to ensure the test strips are compatible with your glucometer. For instance, if you have a OneTouch glucometer, you should also get OneTouch test strips. You’ll also need lancets for your lancing device, though most glucometers come with a few to start.
Here’s a quick checklist of what you’ll need:
Glucometer
Test strips
Lancing device
Lancets
Control solution (optional)
Setting up your meter:
For first-time users, setting up the meter involves:
Setting the date and time
Matching the test strip number to the meter’s settings, if required (adjust using the meter’s buttons if necessary)
Calibrating the meter with a test strip and control solution, if needed
Testing Your Blood Sugar:
Wash your hands with soap and water, which is preferable to using an alcohol swab.
Insert a test strip into your meter. Look for the ready-to-test icon on the screen.
Prick your finger with a new lancet in the lancing device. Adjust the depth setting based on your skin’s sensitivity.
Apply your blood sample to the test strip by gently touching the strip to the blood drop.
Read your results after the meter processes the blood sample.
Clean up by safely disposing of the used lancet and test strip in a biohazard container or a sturdy plastic jug.
Most modern meters have substantial memory and can export data to your phone via USB. Enjoy tracking your blood glucose trends with charts and logs – it’s a great way to actively manage your health!
Dispose safely of the used lancet and test strip in a biohazard container or a thick plastic container with a lid.
Low Carb Diets: A Strategy to Counter Insulin Resistance
Your diet is a vital tool for positively influencing your blood sugar levels. Eating is essential, but making food choices tailored to your body’s needs can significantly enhance your longevity. Here are the best dietary adjustments to maintain low and stable blood sugar:
Avoid liquid calories: Beverages like commercial juices and specialty coffee drinks are often loaded with sugar.
Eliminate sugar wherever you can, and this includes steering clear of artificial sweeteners too.
Increase your fiber intake. Fiber not only keeps you satiated for longer periods, but it also aids in detoxifying your body.
Embrace a whole-food approach. Incorporating a variety of fruits and vegetables into your meals does more than just provide essential vitamins and minerals; it also helps in keeping your carbohydrate intake moderate and your fiber intake high.
Include in Your Diet: Focus on consuming meats, seafood, eggs, above-ground vegetables, and natural fats such as butter, coconut oil, avocado oil, olive oil, and full-fat dairy products.
Avoid in Your Diet: Stay away from sugar, starchy foods like pasta, rice, beans, and potatoes, refined carbohydrates including bread, pasta, bagels, and cereals, as well as processed oils such as corn, cottonseed, soybean, safflower, and sunflower oil.
Use of Berberine for Insulin Resistance:
Berberine, a compound found in several plants, has been increasingly recognized for its potential in managing insulin resistance. It is believed to improve insulin sensitivity and enhance glucose uptake by cells. Berberine works in a way that’s somewhat similar to metformin, a common diabetes medication, making it a promising natural alternative or supplement for insulin resistance management.
Mechanism: Berberine activates an enzyme called AMP-activated protein kinase (AMPK), often referred to as a “metabolic master switch”. This enzyme plays a crucial role in regulating metabolism and has been shown to improve insulin sensitivity, helping to lower blood sugar levels.
Benefits for Midlife Women: Given the increased risk of insulin resistance during midlife due to hormonal changes and other factors, berberine can be a valuable addition to the regimen of those seeking natural interventions. It’s particularly beneficial for women who are either unable to take traditional diabetes medications or are looking for complementary therapies.
Clinical Evidence: Several studies have shown the effectiveness of berberine in lowering blood sugar levels in people with type 2 diabetes. Some research also suggests it may help in weight management and improving lipid profiles, both of which are beneficial for insulin resistance.
In a study, berberine demonstrated an ability to reduce blood glucose levels, aiding in the prevention and treatment of type II diabetes and its related complications, such as diabetic cardiovascular disease and diabetic neuropathy.
Additionally, berberine has shown promising results in influencing glucose-lipid metabolism, reducing inflammation, and improving insulin resistance in individuals with metabolic syndrome.
One notable study highlighted berberine’s efficacy by comparing its effects to the commonly prescribed diabetes drug metformin. Participants took 500 milligrams of berberine two to three times daily over three months. The results showed that berberine was equally effective as metformin in controlling blood sugar and lipid metabolism, leading researchers to regard berberine as a strong oral agent for lowering blood sugar.
Further research reinforces these findings. For instance, a study published in Evidence-Based Complementary and Alternative Medicine revealed that berberine enhances insulin sensitivity by modulating adipokine secretion, which plays a critical role in glucose uptake and lipid metabolism.
Dosage: Berberine is available as a dietary supplement over the counter. The recommended dosage is: 500 mg three times daily (1500 mg per day). If you have a medical condition or are on any medications, including antibiotics, then it is recommended that you speak to your doctor before taking it.
This journey into understanding insulin resistance and the power of low carb diets in midlife highlights the importance of proactive health management. If you’re a midlife woman struggling with insulin resistance, consider how a low carb diet might be beneficial.



 Unlock Your Path to Vibrant Health: A Holistic Guide for Health and Longevity
Unlock Your Path to Vibrant Health: A Holistic Guide for Health and Longevity